
Case Study: Baby Jasmine
This case study was developed for Gaining and Growing by Tracy A.
Delaney PhD, RD, Nutrition Consultant, North Coast Nutrition
- Learning Objectives
- Feeding Team Approach
- History
- Feeding Team Assessment # 1
- Feeding Team Assessment #2
- Feeding Team Assessment #3
- Feeding Team Assessment #4
- Study Questions
- Growth Charts
Learning Objectives:
This case study addresses post discharge nutritional care of VLBW infants. The focus is
on a multidisciplinary team approach to ongoing and developmentally changing feeding
issues. Participants should be able to satisfy the following learning objectives:
- Calculate and plot an infant’s growth parameters using corrected age. Be able to
recognize patterns of growth that indicate growth faltering.
- Gain an appreciation for the importance of the multidisciplinary team approach in
addressing the potentially complex nutritional concerns of post discharge VLBW infants.
- Recognize the diverse array of potential contributors to poor weight gain that should be
addressed in treatment strategies for VLBW infants.
- Understand developmental milestones as they relate to feeding progressions.
- Demonstrate an understanding of key concepts that impact feeding outcomes such as the
feeding environment, oral aversions, the feeding relationship and sensitive periods.
Feeding Team Approach:
Feeding problems are a daily, stressful routine for many families with a VLBW infant.
Feeding issues are usually multi-factorial and complex, involving nutrition, growth, bonding, behavior, developmental readiness, oral aversions, medical complications, financial stress, and time constraints. In order to meet the diverse challenges associated
with feeding issues, the most effective approach is the utilization of a feeding team.
A feeding team includes a multidisciplinary group of professionals, each with a
specialized area relevant to the feeding experience. Feeding teams may include various
combinations of the following: a registered dietitian nutritionist, an occupational, speech, or physical therapist,
a mental health specialist, a nurse, a family resource coordinator, an early intervention
educator, a social worker, and a physician. The family is also a part of the feeding team.
The family helps identify issues that need to be addressed, provides feedback as to the
effectiveness of treatment strategies, and operates as a "reality check"
regarding the practicality of recommendations within the context of the family.
The specifics of a feeding team consultation may vary, but usually include an
assessment of growth, a nutrition evaluation, and a feeding observation that
focuses on oral motor skills, positioning and stability, environmental considerations,
feeding behaviors, medical status and family dynamics. The appointments conclude with
demonstrated treatment strategies that compose the feeding team plan. With each
appointment, the team is able to draw upon the expertise of its members to create, modify
and refine recommendations to optimize feeding and growth outcomes in a dynamic,
integrated, and multidisciplinary manner.
History:
The feeding team has received a referral from a local pediatrician to assess Jasmine,
a former 30 week preemie with a diagnosis of moderate BPD (bronchopulmonary dysplasia).
Jasmine has a chronological age of 4 1/2 months and presents with inadequate weight gain
and "feeding problems."
Medical records indicate that Jasmine had a birth weight of 1450 grams, a birth length
of 40.1 cm, and an OFC of 28.2 cm. She required intubation and mechanical ventilation at
birth. After three days she was extubated and received O2 via nasal cannula
along with a course of steroids. Although initially parenterally fed, Jasmine was
transitioned to gavage feedings within 5 days postnatally using a standard preterm formula
mixed to 24 kcal/oz. At 34 weeks gestation, Jasmine received a combination of bottle and
gavage. At the time of discharge (37 weeks gestation), Jasmine was exclusively bottle-fed
with a standard, iron fortified infant formula (20 kcal/oz). She was discharged with half
a standard daily multivitamin supplement and inhaled bronchodilators prn. Her discharge
weight was 2975 grams, with a length of 48.2 cm and an OFC of 33.5 cm. Since her initial
discharge she has been briefly hospitalized twice with upper respiratory infections
(URI’s).
Feeding Team Assessment #1:
Jasmine was brought to the appointment by her mother, Shari. Shari describes herself as
Jasmine’s primary caregiver, although her husband Don and her mother-in-law, Colleen,
do participate in some of the feedings. Jasmine’s 4-year old brother, Kyle, was at
home with his grandmother during this appointment.
Shari describes the following: "Feeding times are very stressful for
"Jazzy" and me. She will fuss, pull away from the bottle and spit up all of the
time. She tires out before she has had enough formula, and I end up spending an hour
trying to get her to take all of her bottle because I know she isn’t growing enough.
Most feedings end with Jazzy falling asleep and me crying with a half full bottle left in
my hand. I really dread mealtimes, I know she needs the calories but she never seems to
enjoy feeding—it was so much easier with Kyle, he loved taking a bottle, it was our
quiet time together."
Dietary Intake:
Jasmine's formula was recently increased to a 22
kcal/oz preparation based on her physician’s recommendation due to poor weight gain.
Shari, with the encouragement of her mother-in-law, has tried unsuccessfully to introduce
rice cereal by spoon in hopes that it might help Jasmine gain weight.
Diet records indicate the following "typical" feeding routine:
9:00 am |
Rice cereal, a couple bites attempted, crying and spitting
out food 4 oz formula |
1:00 pm |
4 oz formula |
5:00 pm |
Rice cereal, a few bites attempted, crying and spitting out
food 4 oz formula |
9:00 pm |
4 oz formula |
12:30 am |
4 oz formula |
Although difficult to estimate, Shari thinks that Jasmine is probably spitting up about
1/2 oz to 1-1/2 oz per day.
Anthropometrics:
Weight: 3775 g
Length: 55.2 cm
OFC: 37.8 cm
Feeding Environment:
Jasmine is usually fed on the family room couch,
held by her mother. Kyle is also in the room watching TV or singing along with music
videos so that Shari can watch both kids at the same time. Usually the overhead lights are
on to help "brighten" Shari’s mood. Jasmine is usually put in her crib to
finish sleeping after the feeding.
Feeding Observation:
Jasmine is observed to get noticeably irritable as
she sees the bottle pulled out for her feeding. Jasmine looks away and fusses as Shari
brings the bottle to her lips. The bottle has a Nuk nipple, which is broad and flat.
Jasmine’s neck, arms, legs and trunk become hyperextended and she starts arching to
the side during the feeding. Some coughing is observed during sucking pauses. Jasmine soon
tires from the feeding and begins to nod off. Shari is upset, but persistent in her
repeated attempts to get in more formula. She says this is typical, but at home it goes on
for a longer period of time. When Jasmine sucked on the gloved finger of the feeding
therapist, tongue protrusion was noted, which contributed to an inefficient suck. With the
feeding, Jasmine had increases in respiratory rate from 55 breaths per minute (bpm) to 80
bpm and heart rate increases from 140 beats per minute to 195 bpm. Signs of labored
breathing, sternal contractions and fatigue were observed with the feeding, however no
obvious cyanotic related color changes were noted.
Assessment:
Formula intake (including estimated losses from
spitting up) provides energy intake within the standard range (110 kcal/kg). However, this’s current energy needs because she has inadequate growth. Energy needs are estimated to be in the range of
130-140 kcal/kg/day. Fluid goals are met (150 cc/kg). Jasmine’s respiratory status
was significantly stressed during feeding; she could benefit from the addition of
supplemental oxygen during feedings. Jasmine is not developmentally ready for solids by
mouth. She appears to suffer from possible reflux and should also be considered as a
candidate for possible aspiration from reflux. She has behaviors and a medical history
consistent with oral aversions. Jasmine would benefit from evaluation for reflux and aspiration. Based on results of the evaluation, Jasmine might require treatment for reflux or aspiration or perhaps feeding therapy/
encouraging facial and oral play.
Recommendations:
- Increase formula to 26 kcal/oz.
- Discontinue all solid foods by spoon.
- Decrease the length of feedings—try shorter, more frequent feedings to optimize
efficient time of feeding: 15 minutes maximum. Use a timer.
- Provide a quiet feeding environment with dim lights. Perhaps this could be a quiet color
time for Kyle or a time for him to listen to a book tape with headphones.
- Provide proper positioning during feeding, including neck and hip flexion along with
snugly wrapped arms and legs.
- Switch from the broad flat nipple to a firm, straight one with a round cross section to
supply strong pressure along midline to help encourage more efficient sucking patterns.
- Implement strategies to decrease reflux including upright positioning during and after
feedings. Provide 30 degree prone elevated position in
crib by using a foam wedge. Instructions discussed and handouts provided.
- Refer for evaluation for gastroesophageal reflux and aspiration including VFSS (videofluoroscopic swallow study). Consider medications and other treatment approaches based on results.
- Obtain physicians order to add supplemental oxygen during feedings.
- Return to clinic in 4 weeks.
Feeding Team Assessment #2
Jasmine is currently 6 1/2 months, with a corrected age of 4 months. Her family
canceled her appointment last month, but rescheduled for today’s clinic. Since last
seen, Jasmine’s VFSS showed some microaspiration of refluxed formula, although she
appeared safe with thickened liquids. Jasmine is now taking Zantac (ranitidine) and Reglan (metclopramide) for medical
reflux management. Supplemental oxygen has been added during feedings.
Shari notes an improvement with reflux, particularly since starting meds. She estimates
that Jasmine now spits up only "a very small amount, once every few
days—usually in her crib." She has made recommended positional changes during Jasmine's feedings. The family
hasn’t elevated the crib mattress to 30 degrees, but is willing to try now that
things have calmed down a bit. Feedings have become a little less stressful due to time
limitations—but they "still aren’t the highlight of our day." Jasmine
does not enjoy being touched around the mouth or face and the family avoids any extra touch as much
as possible. Shari reports that she has a difficult time getting the nipple into
Jasmine’s mouth to initiate feeds. "With Kyle, some days he would eat a lot and
other days not too much. It never bothered me, I knew it would even out in the end. With
Jasmine, each feeding seems so important, I feel pressure that she takes in a good amount
at each and every feeding."
Diet Records:
- 34 oz/day of 26 kcal/oz formula
- Feeding Time Limit: usually 15-25 minutes per feedings
Anthropometrics:
Weight: 6.25 kg
Length: 62.0 cm
OFC: 41.1 cm
Feeding Observation:
Shari wrapped Jasmine snugly in a blanket and
demonstrated nice hip flexion positioning for the feeding. When the bottle was presented,
Jasmine became fussy, while Shari forced the nipple into Jasmine’s mouth.
Jasmine’s neck was in an extended position and tongue protrusion was noted, however
she did much better when her neck was repositioned with slight flexion. Although
Jasmine’s endurance was much improved, she did show signs of tiring after 15 minutes
and presented clear signs that she was finished. Shari did not pick up on these cues and
continued to feed; she was visibly tense during the entire feeding observation.
Respiratory rate and heart rate remained WNL during the feeding; no coughing was observed.
Assessment:
Energy intake of 885 kcal/day (~140 kcal/kg/d) is supporting
adequate growth at this time. Fluid intake (~160 cc/kg) is adequate. The family appears to
have been overwhelmed by the number of previous recommendations. There has been no
noticeable improvement in terms of Jasmine’s oral aversion.
Recommendations:
- Thicken all formula feedings with oatmeal to prevent microaspiration.
- Refer for ongoing therapy to address oral aversions and tactile hypersensitivity.
Techniques will also be incorporated into all therapy appointments and
at early intervention classes for further reinforcement.
- Watch Jasmine's signals during feedings and try to respond in kind. Slow down, and even
discontinue the feeding as needed based on her cues—do not force her to continue
feeding when she tires. At this point, ~15 minutes is what she can comfortably handle.
- Discontinue multivitamin supplements due to adequate nutritional intake.
- Return for follow-up next month.
Feeding Team Assessment #3
Jasmine’s chronological age is 8 1/2 months. Shari hasn’t tried introducing
any solids and is hesitant to add something new to the feedings. She consistently
includes the oral/facial play routine her therapist recommends.
Shari describes continued frustration over the feeding and acknowledges it is difficult
for her to stop the feeding when Jasmine begins to pull away or nod off. Shari wonders if
feedings will ever feel like a normal, happy part of Jasmine’s life. She notes that a
friend's baby that is at Jasmine’s corrected age is already eagerly eating solids.
During the feeding observation, Jasmine did show resistance during the initiation of
feeding, but once it was underway, feeding was strong and efficient. Proper positioning
was maintained and no evidence of tongue protrusion was noted. Respiratory and heart rates
were WNL. Cues that Jasmine was finished with the bottle-feeding were not picked up on,
and Shari forced the bottle back into Jasmines mouth, even after adequate volumes had been
consumed. Introduction of solids by the therapists at this appointment met with some
resistance, but was tolerated and handled safely.
Assessment:
Diet records indicate formula intake is 44.5 oz/day
providing ~150 kcal/kg/day. Current intake is supporting weight gain of 25 grams per day. Jasmine’s weight is 7.75 kg, length: 64.8 cm and
OFC: 42.9 cm. Shari is not willing to
change feedings at this point, due to ongoing concerns regarding Jasmine’s growth.
Jasmine is developmentally at a 5-6 month age level and is ready to begin introduction of
solids. Jasmine could benefit from increased oral/facial stimulation. Feeding relationship
issues continue to contribute significant stress, strategies to take some of the pressure
off Shari should be explored.
Recommendations:
- Introduce infant cereal 2-3 times daily. Focus on opportunities of exposure, don’t
worry about nutritional contribution of solids at this point. Jasmine’s father and
grandmother will feed Jasmine daily.
- Information regarding nutritional and developmental progressions was discussed and
handouts provided. The family was encouraged to use these as a guide for introducing new
foods and feeding techniques. The importance of capitalizing on "sensitive
periods" was discussed.
- Increase oral/facial play. Additional exercises were demonstrated and handouts provided.
Jasmine’s father and grandmother have agreed to participate in exercises on a daily
basis.
- Importance of the feeding relationship and watching for feeding cues was discussed.
Ellyn Satter’s concept of the division of responsibility was described. Videotapes of
the last two feeding observations were reviewed with Shari. Tapes were provided to take
home for additional viewing at Shari’s request. (She was surprised to see the degree
of struggle that the video showed.)
Feeding Team Assessment #4
At today’s feeding team clinic, Jasmine’s chronological age is 10 1/2 months.
Shari reports a significant decrease in stress now that she is getting more family support
with the therapies and feedings. She is quick to mention, however, that even with these
improvements it still seems like Jazzy does not enjoy mealtimes, although is admittedly
much less resistant. Shari reports that Jasmine will eat a nice variety of foods, similar
to the guidelines provided. However Jasmine is challenged by foods with multiple textures,
and will often spit out lumps. Shari is blenderizing all foods to make them smoother and
increase Jasmine’s acceptance. She worries that they may have hit a plateau in terms
of Jasmine’s ability to eat any textures. "Every time there is any feeding
problem, a little part of me wonders if this is just an off day, or the beginning of a
major backslide."
The feeding observation started with Shari initiating oral stimulation exercises
suggested by the feeding therapist. The feeding confirmed an acceptance for smooth foods and single
texture foods including crackers and teething biscuits. However, when multiple textures
were presented, i.e., smooth foods with very small, soft lumps, the lumps were carefully
spit out. When finely ground crackers were added to pureed foods, however, she hesitantly
ate all that was presented. When cup drinking was attempted, a large amount of liquid fell
from the corners of Jasmine’s mouth. When the juice was thickened with pureed fruit,
better control was demonstrated. There was no choking or gagging with any of the thin or
thickened liquids tried.
Anthropometrics:
Weight: 8.70 kg
Length: 68.2 cm
OFC: 44.2 cm
Assessment:
Intake provides 1250 kcal/day. Solids contribute 15-20% of
total energy. Fluid intake is adequate. Continue formula preparation at 24 kcal/oz and plan to gradually introduce milk from a cup in the next month. Shari agreed that she is ready for this change now that she
is more confident that Jasmine’s growth has improved. Diet records indicate a
developmentally appropriate feeding schedule of meals and snacks, including independent
feeding with teething foods, such as crackers and biscuits. Strategies to gradually
improve tolerance to soft, small lumps should be introduced.
Recommendations:
- Add finely mashed crackers to smooth foods. As Jasmine’s tolerance improves,
gradually increase the size of the cracker crumbs. With time, add more challenging
textures, but do so in a very gradual manner. Consistency is key. The concept of sensitive
periods was again discussed.
- Continue formula preparation at 24 kcal/oz and plan to gradually introduce milk from a cup in the next month. Instructions for transition provided.
- Continue to gradually increase volumes of solid foods. Guidelines provided.
- For improving cup drinking skills, thicken liquids so that they will move slowly and
provide Jasmine an opportunity to learn this new skill. Thickening of liquids can decrease
as drinking skills improve. Do not use commercial thickeners.
- Family encouraged to proceed with feeding changes as Jasmine’s developmental
indicators dictate.
Study Questions
-
Plot Jasmine’s anthropometric measurements on a growth chart. Calculate
Jasmine’s average weight gain since her initial discharge from the hospital at 37
weeks gestation to her initial feeding team assessment? Is her growth adequate and why?
Gairdner and Pearson curve follow.
| Age |
Weight |
Weight Percentile |
Length |
Length Percentile |
OFC |
OFC Percentile |
| Birth |
1450 g |
just <50th |
40.1 cm |
just <50th |
28.2 cm |
50th |
| 37 weeks CA |
2975 g |
just <50th |
48.2 cm |
just <50th |
33.5 cm |
50th |
| 2 months CA |
3775 g |
<10th |
55.2 cm |
just <50th |
37.8 cm |
just <50th |
| 4 months CA |
6.25 kg |
50th |
62.0 cm |
50th |
41.1 cm |
50th |
| 6 months CA |
7.75 kg |
just >50th |
64.8 cm |
50th |
42.9 cm |
50th |
| 8 months CA |
8.70 kg |
just >50th |
68.2 cm |
just >50th |
44.2 cm |
just <50th |
To calculate average weight gain since initial hospital discharge:
The optimal rate of weight gain for premature infants has not been defined. It is common
practice to aim for intrauterine growth rates (15 g/kg/day) and 0.5-1.0 cm/wk in length,
during initial hospitalization. Thereafter, expected rates of growth for term infants,
using corrected age, may be used for comparison. (0-4 months 20-25 g/d; 5-12 months 15
g/d)
Jasmine is gaining an average of 10.4 g/d; this is only half of the minimum
recommended guidelines. In addition, Jasmine is "falling off" her own growth curve. Weight and length were close to the 50th percentile at discharge, but weight fell significantly to
below the 10th percentile at 2 months CA. There is also evidence that her rate of growth for
length may also be slowing. Although VLBW and ELBW infants may not experience catch-up
growth in the first 1-3 years of life, their growth should not slow.
-
Based on the information presented at the initial feeding team assessment, what factors
are likely contributing to Jasmine’s poor growth?
- Increased energy needs due to respiratory distress/desaturation, BPD
- Fatigue/poor endurance: limited intake
- Inappropriately early introduction of solids, displacing formula attempts
- Reflux: losses and discomfort leading to decreased intake
- Aspiration: Increased URI, illness and hospitalization, higher need, lower intake
- Oral aversion: likely due to previous medical experiences, nipple choice likely
exacerbates problems with tongue protrusion, limiting intake
- Inefficient suck-due to tongue protrusion, limiting intake
- Distracting feeding environment with noise, bright lights, TV, sibling
- Hyperextended positioning-reduces intake
- Long feeding times- reinforce negative feeding experience
- Stressful feeding relationship between mom and baby
-
What is Jasmine’s corrected age at the initial feeding team assessment? How would
this information plus the stages of developmental readiness affect your recommendations
regarding introduction of solids?
At 4 1/2 months, Jasmine’s corrected age (CA) is 2 months. She was born at 30
weeks gestation or 10 weeks (2 1/2 months) prematurely. Using CA one can more
appropriately adjust expectations for growth and developmental milestones. Thinking in
terms of corrected age (instead of chronologic age) can help decrease family disappointment regarding their baby's
progress. Depending on the severity of prematurity and
medical complications, the VLBW infant may face delays even when using CA.
As far as introduction of solids, a starting point would be to look at CA. In this
case, 2 months is inappropriately early for introduction of solids. Complementary foods, in the form of
infant cereal, are generally recommended between 4-6 months CA. In addition, the
following developmental milestones indicate readiness for solids:
- Infant can sit with support and has neuromuscular control of the head and neck
- Infant can take food without choking or gagging
- Infant can indicate desire for food by opening the mouth and leaning forward
- Infant can indicate satiety by leaning back and turning away
- Strong extrusion reflex has faded, and infant demonstrates ability to swallow non-liquid
foods, to transfer food from the front of the tongue to the back, and to draw in the lower
lip as the spoon is removed
- Infant exhibits beginning of up and down chewing movements as opposed to sucking
movements with mouth
-
What mixing instructions would you provide to this family for preparing the 26 kcal/oz
formula? Why is method recommended? Would you suggest a liquid concentrate or powdered
formula—why?
Instructions for mixing formula to 26 kcal/oz should likely follow these
recommendations: It is safe to concentrate formulas to 24 kcal/oz and then to add modular
carbohydrate and/or fat products to increase the concentration above 24 kcal/oz up to 30
kcal/oz. Increasing the formula alone above 24 kcal/oz may pose a risk to an infant with
immature kidneys and/or tenuous fluid balance due to the increased renal solute load.
Whenever concentrating formula be sure to check percentage of total calories for
macronutrients for adequacy and assure proper fluid intake for hydration.
Liquid concentrate would be preferred due to the ease of precise measurements,
especially when concentrating formula. Powdered formula scoops have
variable sizes and do not always equal 1 Tbsp. In addition precise
measurements using scoops can be more difficult. Liquid concentrate, however, is more
expensive than powdered formula and may be cost-prohibitive for some families. In that
case, a careful demonstration of formula concentrating instructions would be recommended.
-
What impact can the environment have on the feeding experience?
The feeding environment can either help optimize the feeding experience or
represent a significant source of stress, which can contribute to feeding problems. The
feeding environment is an important component to successful feeding and should always be
evaluated whenever an infant has growth or nutrition issues. Potential sources of stress
within the feeding environment can include bright lights, noise, TV, variations in
ambient temperature and distracting movements of siblings or others. Feeding guidelines
should be provided to help decrease exposure to a stressful feeding environment and
eliminate counterproductive distractions.
-
What "red flags" at the initial feeding assessment indicate potential
aspiration?
- Coughing observed during sucking pauses at initial feeding assessment may indicate
formula ascending into pharynx from gastroesophageal reflux (GER)
- Medical history of two upper respiratory infections (URI) and resulting hospitalizations
within the 11 weeks since the initial hospital discharge
- Avoidance of bottle upon presentation may be related to discomfort of reflux and
aspiration
- Delayed oral/motor skills can increase risk of aspiration cue to poor control and
coordination
- Infants with increased respiratory rate may be at higher risk of aspiration
-
If a highly elevated heart rate and respiratory rate are observed during a feeding, what
might this indicate?
Increases in heart rate >10 beats/min and respiratory rates of 80 breaths/min,
as measured during pauses in sucking, may indicate that the feeding is placing excessive
demands on the infant. If this is the case, the infant may be working too hard to feed
efficiently. Additional support to the cardiorespiratory system, such as supplemental
oxygen or medications and/or nutritional support by way of non-oral supplements may be
needed.
-
What evidence indicates difficulties in the feeding relationship between Shari and
Jasmine? Discuss why an infant with low birth weight might be at higher risk for problems in the
feeding relationship.
Evidence that difficulties exist in the feeding relationship between Shari and
Jasmine include:
- Feeding is described as dreaded and stressful, often ends with mother crying, infant
sleeping
- Feedings are prolonged, around an hour
- Oral aversions make feeding unpleasant for Jasmine, difficult for Shari to provide
nutrition
- Reflux/aspiration/impaired respiratory status causes discomfort, negative reinforcement
of feedings
- Poor reading of feeding cues such as satiety signals
- Force feeding-- Shari feels pressure to provide high amounts of calories with each
feeding
- Fearful outlook of future feeding
- Infants with VLBW may be at higher risk to develop problems in the feeding relationship
due to the following:
- Oral/facial aversions due to experience with prolonged airway intubation or tube
feeding, which can result in lack of infant interest/enjoyment.
- Limited exposure to oral stimulation if fed via nasograstric tube early in life. Lack of
early oral sensory input can lead to hypersensitivity and hyperirritability during
feeding.
- Prolonged feeding times and/or poor feeding endurance results in stress for infant and
feeder.
- Oral motor problems may limit infants self-regulatory abilities (such as sucking to
relieve stress and help reach an organized state), decreasing opportunities for
parent-infant interaction. Preterm infants are often found to have higher rates of
"difficult" temperament in the first months of life. Infant’s birth weight
and temperament at 4 months of age are predictive of mother-infant interaction with
preterm infants.
- Bonding issues due to prolonged hospitalization and medical status
- Postnatal complications can increase stress and interfere with feedings
- Lack of parental confidence regarding feeding
- Increased rates of maternal depression and anxiety with VLBW infants
- Infant perceived as fragile, mothers might feel insecure handling infant
- Growth problems can exacerbate maternal pressure at feedings
- Describe the concept of sensitive periods (developmental windows of opportunity) as they
relate to feeding progressions.
Sensitive periods are developmental windows of opportunity when infants are ready
to accept advances in taste, texture, and/or feeding methods. If these "sensitive
periods" are missed and the corresponding feeding experience is not provided, it may
be difficult for the feeding development to progress normally. Often a child who missed
feeding exposures during these sensitive periods seems to get stuck at a certain level of
feeding progressions and has a difficult time making the next developmental change. This
is especially important for babies with prolonged nasogastric or gastrostomy feedings.
Some type of ongoing oral motor program is needed for tube-fed children, even if they are
not taking foods by mouth at that time.
-
What are the developmental stages that indicate it is appropriate to start introducing
finger foods? What developmental milestones show readiness for cup drinking?
Finger Foods: Child should already have developmental indicators for pureed solid
foods and
- Infant can sit independently and maintain balance while using hands to reach and grasp
objects.
- Infant grasps large pieces of food such as thick, dry, infant toast, in a palmar grasp
Cup Drinking: Child should have demonstrated developmental indicators for pureed solid
foods, finger foods and
- Infant exhibits ability to control size of sip and to manipulate liquid bolus to back of
mouth and swallow without choking or gagging
Growth Charts
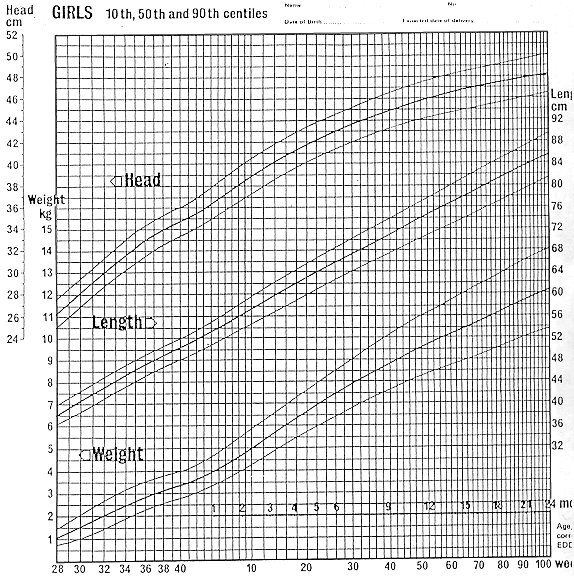
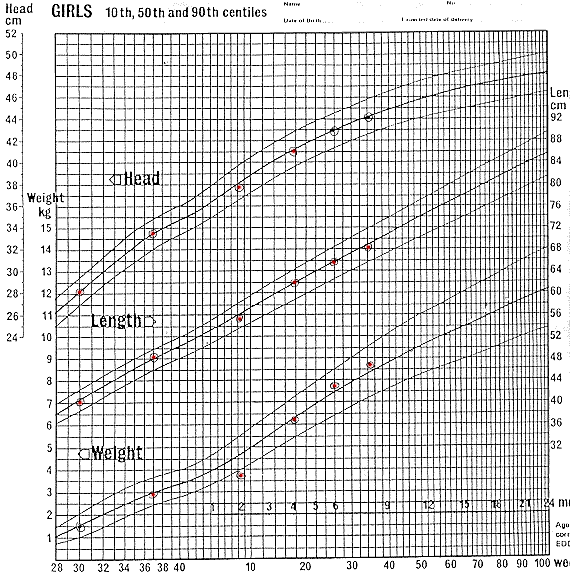
Girls Growth and Development Curve
Prepared by Drs. D. Gairdner and J. Pearson. Published in Archives of Disease
in Childhood 1971.
More information contact: growing@uw.edu
Page reviewed: March 24, 2015

